Hospital tension (or stress) is commonly understood to mean overuse or overburdening of available resources, whether material or human. However, it is undeniable that, whatever the trade, working under high tension can be unpleasant.
If the word Tension has been on the lips of hospital care workers for many years, it has recently contaminated political leaders who could not ignore it any longer, considering the health crisis generated by the Coronavirus. Indeed, the anger of the French emergency doctors — which led to 6 months of labor strikes in 2019 — was more than legitimized in the first quarter of 2020.
So what are the technological levers to counter hospital tension, which continues to grow over the years?
The nerve center of tension is the emergency room (ER), which receives unscheduled patients 24/7 by definition. However, a large intake volume is not the decisive parameter for characterizing the load on this unit. On average, 1 out of 3 patients presenting himself to the ER will require hospitalization for illness or accident, in particular for postoperative convalescence. Every hospitalization requires finding a bed and emergency units ventilate patients on almost all downstream wards at random times. This impermanent nature is often perceived as a disruption by the host service, which sometimes goes as far as refusing patients even when beds are available, to keep them for more “conventional” cases. Patients should then be placed on hold in the ER or “hosted” in a temporary or even inadequate service. In short, it is less the admissions than the slowness of hospital discharges that are problematic.
We have all been to the ER some day and felt that we were waiting too long and/or not informed enough. Well, this sometimes reflects a fragilized upstream/downstream coordination that clogs up the emergency department, in addition to difficult cases to handle. The incessant phone calls between emergency doctors or health care managers and hospital services can accumulate hours of backlog over the course of a day.
Measuring tension within a hospital
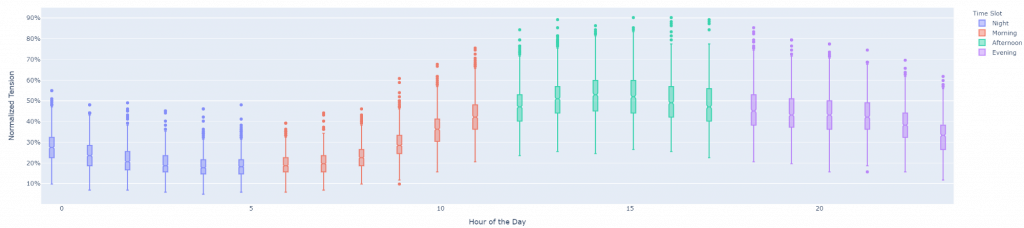
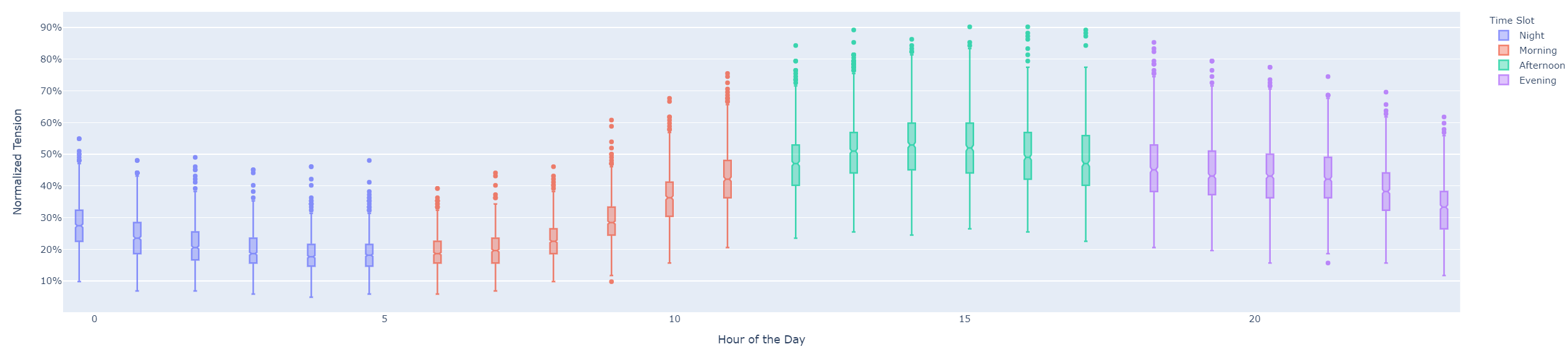
There are several indicators of the hospital tension, the most basic being the number of patients present in the department at any given time. It is measured in terms of incoming and outgoing flows during an hour, for example. As the ward is always open and never completely empty, the analysis of tension over a time period requires several measuring points, or to know the patient count with the largest possible historical depth, preferably since the opening of the ward. The calculation is then a cumulative sum of: the admission-discharge difference. An analogy can be made with the balance of your bank account that results from a series of debits and credits over a period of time. A “high tension” is then observed in a hospital when the admissions are much higher than the discharges, which indicates a majority of patients staying in the ward for a long time. The Figure 1 shows a statistical profile of tension at an emergency unit by time of day (accumulated over a year). We can see that the variability and intensity is statistically greater past noon.
A subtler and more relevant measure requires to take into account the available human resources, as a high influx can always be managed by a sufficient medical contingent. A simple way of weighing the tension is then to calculate the average number of patients per caregiver, which can be broken down by care assistant, nurse and doctor if necessary. In an ideal world, this indicator would remain constant over hours and days, thanks to an optimal and dynamic sizing of teams. However, this requires a forward-looking view of the mid-term situation at least, which is not easy in such an uncertain environment.
Predicting unplanned activities
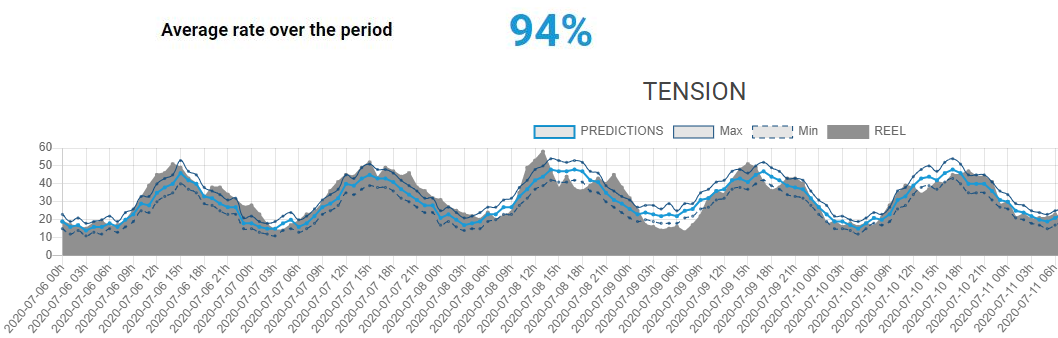
In this context, a predictive system such as CALYPS Saniia can be of great help. Thanks to Artificial Intelligence (A.I.) and Deep Learning, we are able to predict several days in advance the upcoming tension profile, hour by hour, with an accuracy over 90%. This level of performance is ensured by the expertise of our Data Science Team, who implements the latest academic developments in Machine Learning. We integrate in our forecast algorithms numerous indicators including external data (weather, events, particular days, news…) in order to predict admissions as well as hospital discharges and thus in-depth tension (see Fig 2 below).
With such a tool, it becomes possible to predict the expected number of patients per caregiver, according to a given weekly team planning. The head of the unit has then a tool enabling the test of resources sizing and its impact for next days. The level of assistance can be further increased by asking the system to suggest an optimal schedule, taking into account the personal constraints of caregivers. This avoids under-staffing, but also over-staffing in periods of low needs.
Additionally, during the course of a day, our system is able to follow the entire path of the patient to the emergency room. We predict the next events to come (imaging, laboratory, discharge, hospitalization…) and when they will take place. For patients requiring hospitalization, we calculate in near real time the optimal bed in which the patient should be placed.
Calyps.ai acts as an automated referee between the emergency and downstream services, while waiting for validation by doctors. Thus, Calyps offers a real logistics optimization tool to give back time to caregivers for what really matters : treating patients.